For millions, persistent back pain is more than a fleeting inconvenience; it’s a daily reality that can diminish quality of life, limit mobility, and cloud the simplest joys. The quest for relief often leads down a confusing path of conflicting advice, from quick fixes to invasive procedures. This review aims to cut through the noise, examining common approaches to managing lower back pain with a clear-eyed perspective on their effectiveness and practical application.
Understanding the Landscape of Back Pain
Before exploring solutions, it’s crucial to understand the nature of the problem. Lower back pain is rarely a single condition but a symptom with diverse potential causes. These can range from muscular strains and ligament sprains to issues with spinal discs, joints, or nerve roots. A proper diagnosis from a healthcare professional is the essential first step toward a targeted and effective management plan.
Chronic pain, typically defined as lasting longer than three months, often involves complex interactions between physical structures, nervous system sensitization, and lifestyle factors. This complexity is why a one-size-fits-all solution rarely exists, and why a multi-faceted strategy is frequently the most successful.
Common Conservative Approaches: A Closer Look
The initial management of lower back pain, especially when acute, overwhelmingly favors non-invasive methods. These approaches focus on reducing inflammation, improving function, and building resilience.
Physical Activity and Targeted Exercise
Contrary to outdated advice for strict bed rest, controlled movement is now a cornerstone of back pain management. Inactivity can lead to muscle weakening and stiffness, potentially prolonging discomfort. The goal is to find a balance between movement and rest.
Effective programs often include:
- Core Stabilization: Exercises that strengthen the deep abdominal and back muscles (the “core”) provide dynamic support for the spine, reducing strain on passive structures.
- Aerobic Conditioning: Low-impact activities like walking, swimming, or using an elliptical machine promote blood flow, reduce stiffness, and can aid in weight management—a key factor for spinal health.
- Flexibility and Mobility Work: Gentle stretching for the hamstrings, hip flexors, and lower back can alleviate tension and improve range of motion.
Manual Therapies and Professional Care
Hands-on techniques provided by licensed professionals can be valuable components of a comprehensive plan. These practitioners assess movement patterns and apply specific interventions.
- Physical Therapy: A physical therapist can design a personalized exercise regimen, provide manual therapy, and educate on proper body mechanics for daily activities.
- Chiropractic Adjustments: Spinal manipulation aims to improve joint mobility and may offer relief for some types of acute, uncomplicated lower back pain.
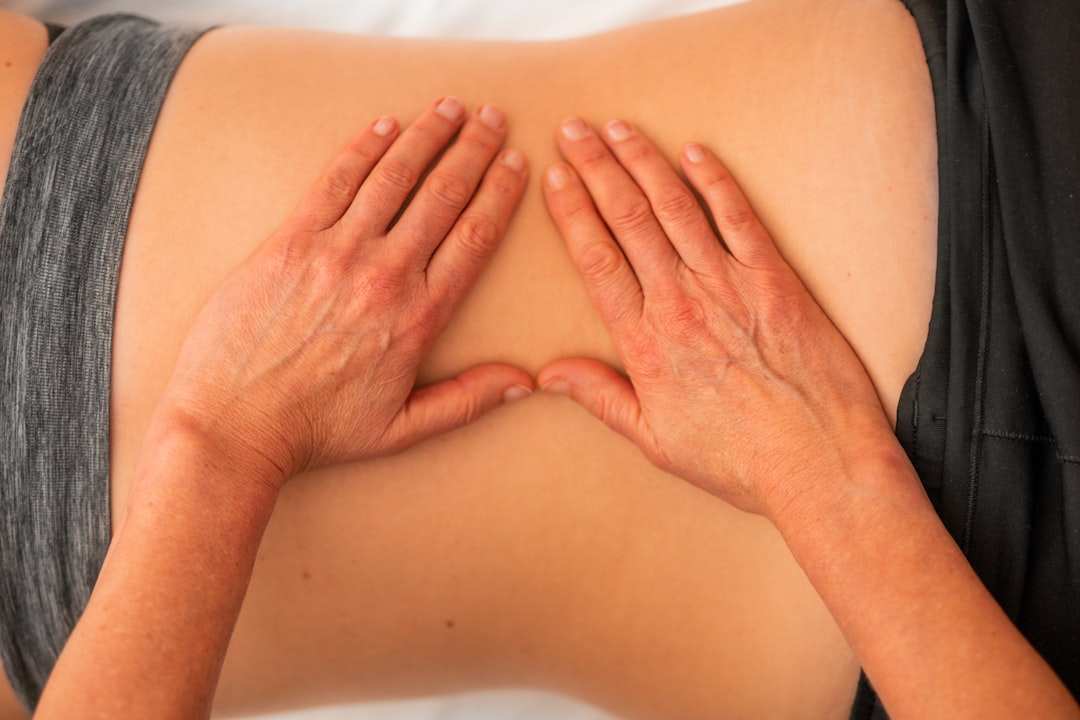
- Massage Therapy: Therapeutic massage can help reduce muscle tension, improve circulation, and promote relaxation, which is beneficial for pain management.
Mind-Body Techniques and Pain Education
Modern pain science emphasizes the brain’s role in perceiving and modulating pain signals. Techniques that address this connection are gaining strong support in clinical guidelines.
- Cognitive Behavioral Therapy (CBT): CBT helps individuals identify and change negative thought patterns and behaviors associated with chronic pain, reducing its perceived intensity and impact.
- Mindfulness and Meditation: These practices cultivate a non-judgmental awareness of the present moment, which can help reduce the stress and anxiety that often amplify pain.
- Pain Neuroscience Education: Understanding how pain works—that it is an output of the brain based on perceived threat, not just a measure of tissue damage—can be profoundly empowering and reduce fear.
Medical and Interventional Options
When conservative measures provide insufficient relief, or when a specific diagnosable condition is present, medical interventions may be considered. These should always be pursued under the guidance of a physician.
Pharmacological Management
Medications are typically used for short-term symptom control or as part of a broader plan. Common categories include:
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Medications like ibuprofen or naproxen can reduce inflammation and pain.
- Muscle Relaxants: These may be prescribed for short-term use during acute muscle spasms.
- Topical Analgesics: Creams, gels, or patches applied to the skin can provide localized relief with minimal systemic side effects.
Interventional Procedures
For targeted pain stemming from a specific nerve or joint, a specialist may recommend procedures such as epidural steroid injections or nerve blocks. These are diagnostic and therapeutic tools, not permanent solutions, and their effectiveness varies.
Evaluating Lifestyle and Ergonomic Factors
Daily habits and environments play a monumental role in spinal health. Lasting relief often requires addressing these foundational elements.
- Posture and Ergonomics: Optimizing your workspace, using supportive seating, and practicing neutral spine alignment during activities can prevent cumulative strain.
- Sleep Hygiene: Quality sleep on a supportive mattress is critical for tissue repair and pain modulation. Finding a comfortable sleep position, often on your side with a pillow between your knees, can help.
- Nutrition and Hydration: An anti-inflammatory diet rich in whole foods and proper hydration supports overall tissue health and can influence inflammatory processes related to pain.
- Stress Management: Since stress directly tenses muscles and heightens pain perception, integrating regular relaxation practices is non-negotiable for chronic management.
Synthesizing a Personalized Path Forward
The most effective strategy for managing lower back pain is rarely a single treatment but a coordinated combination of the approaches reviewed. Success depends on personalization—what works for one individual’s specific condition, lifestyle, and goals may differ for another. The journey from persistent discomfort to improved function involves patience, consistency, and often, professional guidance to build a sustainable plan. The key takeaway is that while back pain is common, enduring it without hope is not necessary. A modern, multi-modal approach focused on active rehabilitation, education, and lifestyle integration offers a realistic pathway to reclaiming comfort and mobility.

Leave a Reply